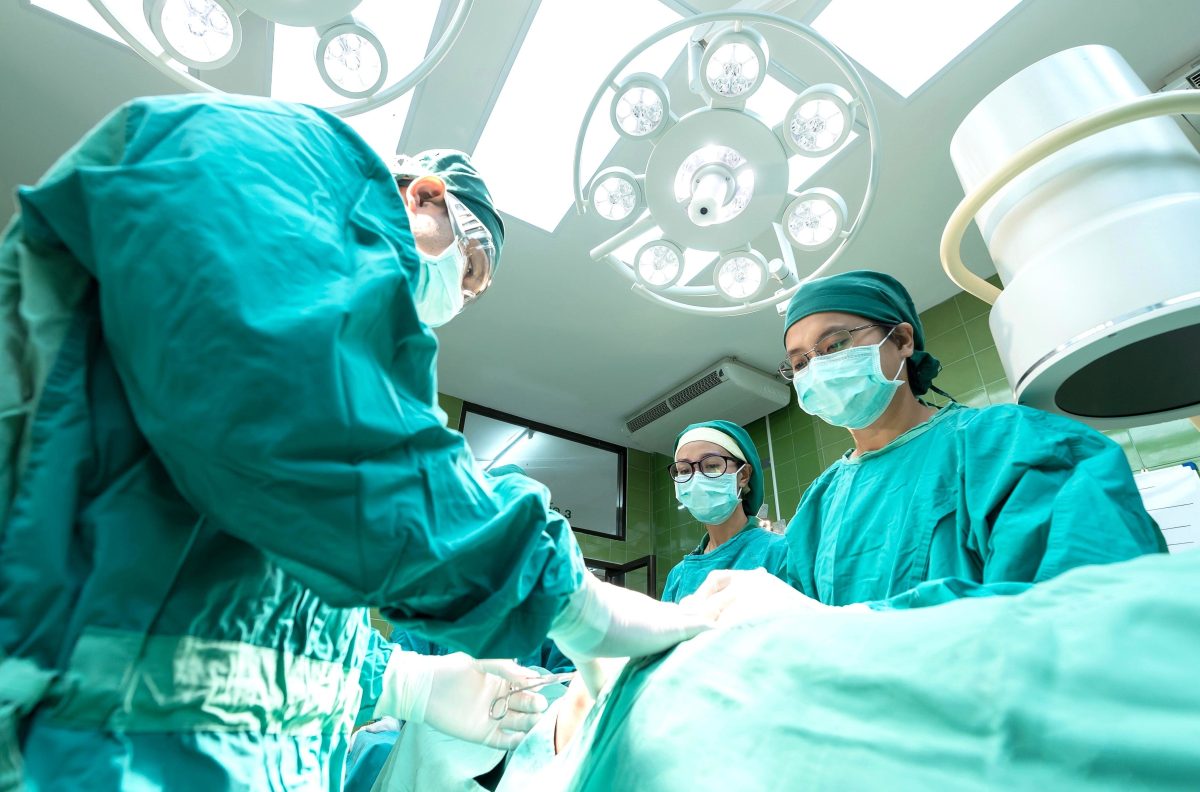
Artificial intelligence is no longer a futuristic promise in the field of healthcare. In 2026, it has become a concrete tool, used every day by thousands of doctors around the world to detect diseases earlier, reduce diagnostic errors, and improve the quality of care. This silent revolution is profoundly redefining our relationship with medicine.
A technology that reads where the human eye may fail
Medical diagnosis has always relied on observation, experience, and interpretation. But these human qualities have their limits: fatigue, the volume of data to process, and the rarity of certain pathologies that makes them difficult to recognize. It is precisely in these areas of fragility that AI excels.
Deep learning algorithms are now capable of analyzing thousands of medical images — X-rays, MRIs, CT scans, histological sections — in a matter of seconds, with a precision that sometimes surpasses that of the most experienced specialists. In 2026, several clinical studies have confirmed that some AI models detect breast cancer on mammography with an error rate below 3%, compared to an average of 5 to 7% for a human radiologist working alone.
Concrete advances across multiple specialties
The impact of AI is not limited to a single discipline. Today it touches many medical specialties:
- Oncology: early detection of breast, lung, skin, and colon cancers has been considerably improved thanks to AI-assisted image analysis and genomics tools.
- Cardiology: algorithms analyze electrocardiograms in real time and detect rare arrhythmias that even an experienced cardiologist might miss on a tracing of a few seconds.
- Ophthalmology: diabetic retinopathy, the leading cause of preventable blindness worldwide, is now automatically screened from a simple digital retinal image in many countries.
- Dermatology: consumer applications allow patients to photograph a skin lesion and receive a preliminary assessment within seconds, even before consulting a doctor.
- Psychiatry: language analysis models and facial micro-expression tools are beginning to be used for early screening of severe depression and bipolar disorders.
AI as an assistant, not a replacement
A frequently expressed concern is that doctors will be replaced by machines. In reality, the practical experience of 2026 tells a very different story. AI acts as a benevolent second opinion — it draws the clinician's attention to a suspicious area, suggests a differential diagnosis, or alerts on an abnormal result that the workload might have caused to go unnoticed.
"Artificial intelligence does not replace the doctor. It allows them to devote their energy to what the machine cannot do: listen, reassure, and decide together with the patient."
This collaborative model is now the consensus in the medical community. The best-performing tools are those that augment the practitioner's intelligence without bypassing them. And the results speak for themselves: in hospitals that have integrated these tools, diagnostic delays have been reduced by 30 to 50% for certain pathologies, and false negative rates have significantly decreased.
Major ethical and regulatory challenges
Despite these impressive advances, the integration of AI in medicine raises fundamental questions that our societies must address.
The first is that of responsibility: if an algorithm makes an error that causes harm to a patient, who is liable? The doctor who trusted the machine? The software publisher? The hospital that chose to adopt it? European medical law is still adapting to this new reality.
The second is that of algorithmic bias. AI models learn from historical data. Yet this data often reflects existing inequalities: certain pathologies may be less well recognized in women, older people, or populations with darker skin if they were underrepresented in training datasets. Correcting these biases is an essential task, still largely ongoing.
Finally, the issue of medical data privacy remains central. Training a high-performing model requires millions of anonymized patient records. In France, the Health Data Hub — although already operational — is still the subject of intense debate about the guarantees offered to citizens.
France in the global AI healthcare race
France holds a notable position in this field. Public and private investment in digital health exceeded 3 billion euros in 2026. Startups such as Cardiologs (ECG analysis), Gleamer (radiological imaging), and Owkin (AI and cancer research) are establishing themselves internationally and showcasing French expertise.
The university hospitals in Paris, Lyon, and Bordeaux are experimenting with medical decision support systems in their emergency and radiology departments, with promising results in terms of speed of care and staff satisfaction.
And tomorrow?
The coming years promise to be even more transformative. Predictive medicine — that is, the ability to anticipate the onset of a disease before the first symptoms even appear — is one of the most ambitious frontiers of medical AI. By combining genomic data, lifestyle, environment, and medical history, some models are already able to predict with unprecedented precision the risk of developing type 2 diabetes, cardiovascular disease, or certain forms of cancer within five to ten years.
The era of personalized and predictive medicine is opening. And artificial intelligence is its cornerstone.
 English
English  French
French  Spanish
Spanish  Chinese
Chinese  Japanese
Japanese  Korean
Korean  Hindi
Hindi  German
German  Norwegian
Norwegian