In February 2025, an infant named KJ made history in medicine. Born with a rare and potentially fatal genetic disease, he became the very first human being to receive a fully personalized CRISPR gene therapy. One year later, the results exceed all expectations and open a revolutionary path for millions of patients worldwide.
A rare disease with devastating consequences
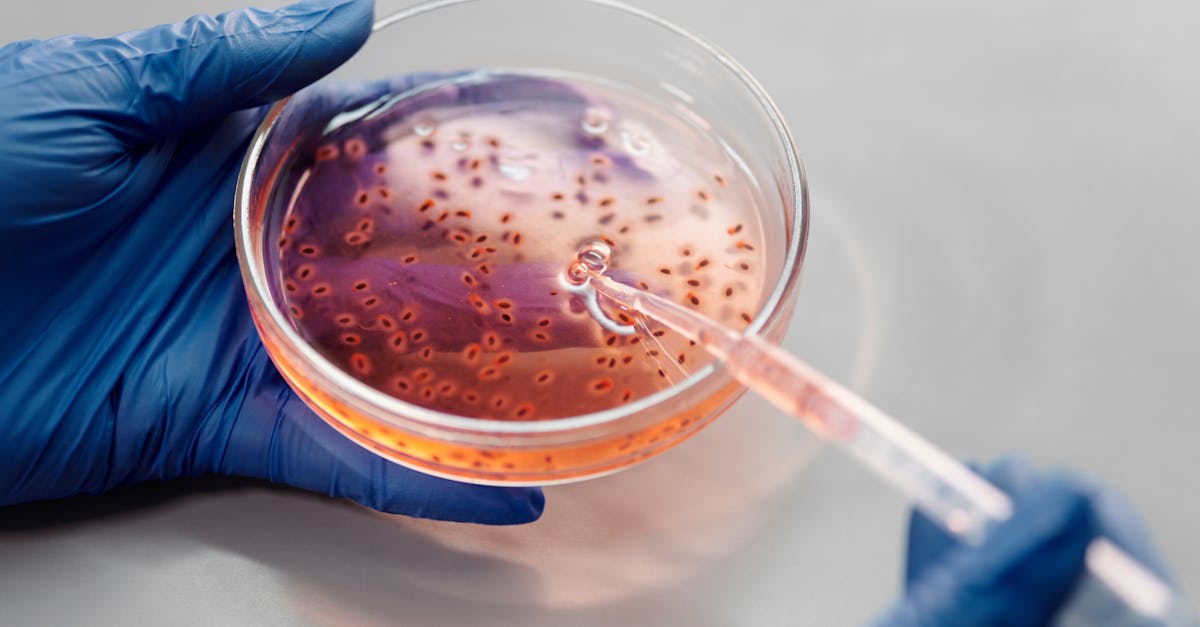
KJ was born with a deficiency in carbamoyl phosphate synthetase 1 (CPS1), a hereditary metabolic disorder affecting approximately 1 in 1.3 million births. This enzyme, essential to the urea cycle in the liver, normally eliminates the ammonia produced by protein breakdown. Without it, ammonia accumulates in the blood and can cause irreversible brain damage or even death.
From birth, KJ had to follow an extremely low-protein diet and take powerful nitrogen-scavenging medications to maintain tolerable ammonia levels. At just five months old, his condition was so precarious that he was placed on the liver transplant waiting list — a major surgical procedure, risky, and with unpredictable availability for such a young patient.
Six months to create a tailored treatment
It was at the Children's Hospital of Philadelphia (CHOP) that the team of Dr. Rebecca Ahrens-Nicklas took on an unprecedented challenge: to design, manufacture, and administer a personalized gene editing therapy in just six months. The technology used, called base editing, is an evolution of classical CRISPR. Rather than cutting DNA like molecular scissors, base editing modifies a single letter of the genetic code with surgical precision, without causing a double-strand break.
The treatment was encapsulated in lipid nanoparticles — the same technology used for mRNA vaccines — in order to deliver it directly to KJ's liver cells. The goal: to correct the mutation responsible for the CPS1 enzyme dysfunction and partially restore its ability to eliminate ammonia.
Encouraging results one year later
On February 25, 2025, KJ received his first infusion. Two additional doses followed in March and April. As Dr. Ahrens-Nicklas noted: "While this treatment is not a definitive cure, after three infusions, KJ has tolerated it well without serious side effects."
One year later, the progress is remarkable. KJ walks, talks, and reaches the expected developmental milestones for his age. His diet has been enriched with protein, and the doses of nitrogen-scavenging medications have been reduced. Even during episodes of childhood illness — critical moments when ammonia can spike — his levels remained under control.
A regulatory revolution to accelerate access
KJ's story does not only transform medical research; it also influences regulation. On February 23, 2026, the American FDA announced a new approval framework called the "plausible mechanism". This mechanism allows personalized therapies to be authorized based on only 5 to 10 patients, rather than the hundreds usually required in traditional clinical trials. A decisive step forward for ultra-rare diseases, where it is sometimes impossible to gather enough patients for a traditional trial.
The CHOP team plans to submit a Phase I/II clinical trial application in 2026 for an expanded platform covering several urea cycle disorders. The GTIMD (Gene Therapy for Inherited Metabolic Disorders) program is already exploring applications for organic acidemias, fatty acid oxidation defects, and phenylketonuria.
A model for the medicine of tomorrow
What makes KJ's case truly revolutionary is not just the therapy itself, but the model it inaugurates. Until now, developing a drug took an average of ten to fifteen years and cost several billion dollars. Here, a tailored treatment was created in six months for a single patient. If this process can be industrialized and made accessible, it is the entire field of rare disease medicine that could be transformed.
A key scientist from the team that treated KJ launched a startup in January 2026, Aurora Therapeutics, with the ambition of democratizing the production of personalized CRISPR therapies. The goal: to reduce costs and timelines so that every patient with a rare genetic disease can one day benefit from a treatment designed specifically for their mutation.
The hope of families and the call to action
KJ's parents, Kyle and Nicole Muldoon, have become advocates for gene therapy research. Nicole stated: "Lawmakers can make this possible by investing in research and expanding access to care." Their testimony reminds us that behind scientific advances, there are families for whom every day counts.
It is estimated that more than 7,000 rare genetic diseases collectively affect between 300 and 400 million people worldwide. For the vast majority of them, no specific treatment exists. The approach inaugurated with KJ could, ultimately, offer a glimmer of hope to each of these patients.
Baby KJ's story is not only a medical feat. It is the signal that medicine is entering a new era — one where the treatment is designed for the patient, not the other way around. A silent revolution, letter by letter, in the great book of our DNA.
 English
English  French
French  Spanish
Spanish  Chinese
Chinese  Japanese
Japanese  Korean
Korean  Hindi
Hindi  German
German  Norwegian
Norwegian